If you experience pregnancy-related pelvic girdle pain or are a professional who encounters patients with pelvic girdle pain, you will find evidence-based information here.
Pelvic girdle pain can affect all pregnant people, but most recover during the postpartum period. Some individuals may experience pelvic girdle pain for many months after giving birth. It is challenging when the pain becomes so intense that it hinders daily activities. Here, we have gathered information about pelvic girdle pain and tips on how to cope, we hope you find it beneficial.
If you experience pregnancy-related pelvic girdle pain or are a professional who encounters patients with pelvic girdle pain, you will find evidence-based information here. Pelvic girdle pain can affect all pregnant people, but most recover during the postpartum period. Some individuals may experience pelvic girdle pain for many months after giving birth. It is challenging when the pain becomes so intense that it hinders daily activities.

Here, you will find several short informational films with evidence-based information for those experiencing pelvic girdle pain and those around them. They are also relevant for healthcare professionals. These films provide guidance on using the body in a way that reduces pain levels and prevents prolonged pain. In addition, they demonstrate everyday activities and share useful knowledge that enhances your understanding of the body’s functions and encourages self-care.
The films are equally accurate and useful for you, regardless of whether you are currently pregnant, have recently given birth, or have lived with pelvic girdle pain for several years. Following the advice in the films lays the foundation for increased physical activity. Small adjustments in how we use our bodies can have a significant impact on pain and functionality, making it possible to participate more actively in family life, work life, and other social activities.
The films are based on clinical experience and research-based knowledge and can be used by both healthcare professionals and patients themselves. The project was carried out in collaboration with the Norwegian Physiotherapy Association’s Women’s Health Group. Physiotherapist and researcher at Oslo University Hospital, PhD Britt Stuge, is responsible for the content and is the instructor in the films. She provides evidence-based advice, coping strategies, and invalidation of ineffective advice or approaches that could worsen the condition.
We recommend starting by watching the film «Pelvic Girdle Pain Explained by FORMI» as it lays the foundation for understanding the background of the instructions given in the other films. Feel free to watch one film at a time and work with them over time; with patience, you can create changes. Remember, small ripples can create big waves.
Read more about pelvic girdle pain at the bottom of the page. Good luck!
Patients with pelvic girdle pain are advised to receive guidance on using their bodies appropriately and that exercises to raise awareness of the pelvis are crucial. What this means is not always obvious, and not everyone has access to a practitioner with this expertise where they live. Both patients and practitioners seek information about this. Therefore, through funding from the Dam Foundation, LKB has created a series of films demonstrating various movement patterns to prevent and reduce pain levels for those affected by pelvic girdle pain.
The film will give you insights into how pelvic girdle pain progresses for women during childbirth. The tips in the film are relevant and useful both before and after giving birth. The film is produced by the Research and Dissemination Unit for Musculoskeletal Health (FORMI) at Oslo University Hospital (OUS) in collaboration with the Norwegian Association for Female Pelvic Joint Health (LKB), researchers from the orthopedic clinic at OUS, and the Norwegian Institute of Public Health.
The film provides examples of how to walk in a relaxed manner, use your feet, and adjust your step length to avoid provoking pain.
The film demonstrates how to sit, vary sitting positions, sit with legs wide apart, half-cross-legged, and in the opposite direction on a chair. It also shows how to sit down and stand up from the chair with minimal pain.
The film illustrates how to stand and shift your center of gravity to reduce pain.
The film presents good resting positions, how to rest effectively, and find comfortable resting positions using pillows while lying on your side or your back.
The film highlights what to be aware of and how to exercise effectively with pelvic girdle pain to reduce pain and avoid exacerbation.
Read about this film project and LKB on the poster to 11th Interdisciplinary World Congress on Low Back & Pelvic Girdle Pain
What to expect during a pregnancy
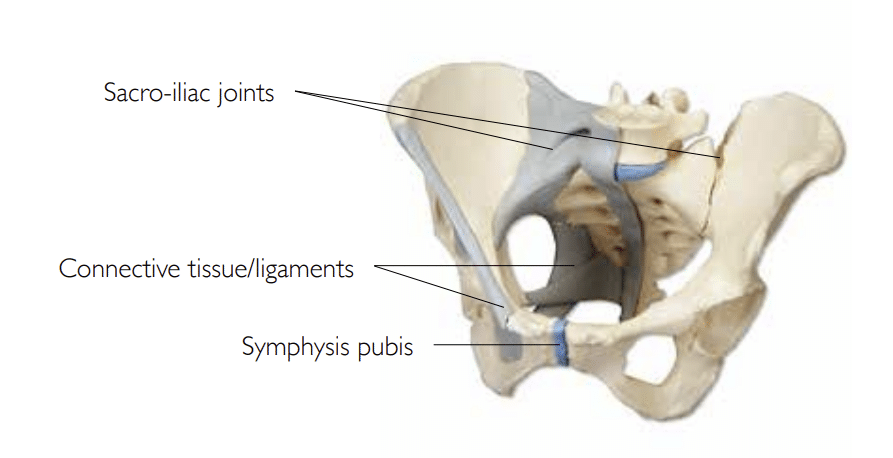
There are three big joints in the pelvis: two sacro-iliac joints at the back, and the symphysis pubis, a joint with a cartilage disc, at the front. These joints are tightly connected by strong ligaments that prevent movement in the pelvis.
A hormonal process that occur in all pregnant women causes the ligaments to become more elastic, thereby making the pelvis more flexible. This is known as physiological pelvic girdle relaxation. As the pregnancy progresses, the woman naturally puts on weight, and the ligaments, which have already become more elastic, are less able to withstand the extra strain.
Do you experience:
- Pain when you walk, stand or sit?
- Pain when you go up or down stairs?
- Difficulty getting up from a sitting position?
- Pain when you try to turn over in bed?
- Pain that makes it difficult to cope with your everyday chores?
You might experience pregnancy-related pelvic girdle pain. The pain can be at the symphysis pubis joint in the front and/or at the back over one of or both the sacro-iliac joints. We recommend you to get a proper exam by a qualified health practitioner to rule out other causes for your pain before you take use of any of the following advice on coping with pregnancy-related pelvic girdle pain.
Your body is designed for movement
Movement is good for the body, and for the pelvic joints. That is why it is important to stay active. Sedentary work or working in one position for a long time can provoke pain. At the same time, it is important to relieve the strain on the pelvic joints in order to prevent the pain from getting worse.
Alternating between activity and rest tends to relieve the pain. Try to find a resting position that suits you. While resting will not cure the condition, you can benefit from good quality rest and thereby cope with activity better. Try to be optimistic and focus on the fact that the condition is not dangerous. The belief that you will get better, combined with physical activity, stimulates the body’s ability to heal itself.
Fresh air and physical activity are good for everyone. The level of exercise should be adapted to suit you and your functional abilities. A physiotherapist can provide professional guidance.
Relaxation
Living with pain and restrictions can be a major stress factor, and the body usually reacts by becoming tense. Over time, this tension can lead to strained, tight and painful muscles. Tension can aggravate pain or create new pain. It is possible to suffer from muscle tension without realising it. The body remains tense at night while you are asleep, when you are active or even when you are enjoying yourself. Relaxation is a collective term that describes various techniques and approaches that can help to reduce tension in the body. Relaxation is an aid to self-help, and promotes mental and physical well-being. Relaxation is something that everyone can learn. There is a lot of information available about relaxation and various techniques and methods. Put some time aside for yourself in a quiet space, as little as five or ten minutes can make a big difference. Most people have to practise a little before they feel the benefit of relaxation, but practice really
does make perfect. Relaxation can make an important and valuable contribution towards improving your quality of life.
Relief
- Try to move as naturally as possible.
- Use your body sensibly.
- Take a rest before you have to, even a short rest can be enough.
- You may have to go on sick leave for short periods.
- Use a support belt, support tape or, if necessary, crutches to reduce the strain.
- Let people know what you need help with. Don’t be afraid to accept help from the people around you.
- Talk to your GP about your needs during and after the pregnancy and birth.
- Also ask the midwife services, health centre and ,if in Norway, NAV (the Norwegian Labour and Welfare Service) for advice. They can help you find out what options are available for adaptation and practical help at home.
Good resting positions:
- Lie on a surface that you find comfortable, such as a pressure-relieving mattress.
- Lie on your side, with a long pillow in front of your chest and tummy and between your thighs, calves and
ankles. Support your whole leg. - Lie on your back with a pillow under your knees and the lower part of your bottom. Your whole body
should feel relaxed. - Sitting backwards on a chair, leaning on the back of the chair, can be very beneficial.
Coping strategies:
- Stand with your weight spread evenly across both feet.
- Don’t carry children on your hip.
- Lift sensibly. Leave the heavy lifting to others. Arrange things so that you can reach your children at a comfortable working height.
- Use a backpack, and when carrying things in your hands, carry the same amount of weight in both hand.
- Wear good shoes, and use spikes in winter.
- When you go for a walk, remember that there and back again is twice as far.
- Change your position often; you’re allowed to fidget!
- Many find that it helps to keep their legs together when they turn over in bed or get in and out of the car.
- Sexual positions can be painful. Use your imagination and explore different positions.
- Get help to adapt the way you carry out everyday movements and chores. Simple things like how you sit, stand or walk, wipe the table, prepare food or make the bed can often be the reason why your pain isn’t going away. Ask to
be referred to a physiotherapist to learn how to use your body sensibly, and, if necessary, for treatment. - Find a therapist who shows respect for the challenges you face, and who you can trust.
- A support belt or support tape can be useful. Use it as needed, but not for too long at a time.
- Take your partner, a close friend or a relative to the treatment sessions and examinations, so that you can get information together.
- Contact the maternity ward well in advance to make preparations for the birth and your stay on the post-natal ward. Make good use of the months before the birth to find positions that you can relax in. Also try out positions
that you think you would like to give birth in, so that you are familiar with them when the time comes. - Lower your own and other people’s expectations and requirements of you. You are the one who have to set the limits
Psychological factors
Pelvic girdle pain in and around the pelvic joints is a musculoskeletal condition. Having persistent and intense pain over
time has an effect on people. Pain often affects your sleep, which means that you become run-down and less able to cope during the day. This makes most people tired, and can affect your mood and your ability to cope with pain.
Plan how best to use your strength during the day. Set aside time for self-care and pleasant experiences. These are important things that will help you to cope and enjoy life.
Why does it hurt?
It is often difficult to establish where the pain is coming from or how it arises. During pregnancy, the tissue connecting a woman’s joints becomes more elastic, which means that the ligaments stretch more, and this can result in pain. There are several structures in and around the pelvis that can cause pain at the same time. The location of the pain varies from woman to woman: it can be over the symphysis pubis at the front, over one or both of the sacro-iliac joints at the back,
in the lower back, around the bottom, in the groin, in the hips, and down one or both legs.
Even if it isn’t possible to determine exactly what causes the pain, the pain you are feeling is real. Pain in and around the pelvic joints can be extremely severe. The muscles can become ‘knotted’, and it feels as if they are cramping.
These pains are very rarely dangerous. Try to think of your pelvis as a sprained ankle. Don’t provoke the pain over and
over again, day after day – that might just make the situation worse. It is much better to pay attention to your body’s signals in order to prevent the pain from developing and becoming chronic. Relieving strain and using your body sensibly will relieve the pain and prevent long-term symptoms.
Will I get better?
The vast majority of women who experience pregnancy- and birth-related pelvic girdle pain will get better, with or without treatment. The condition reoccur in some people, and others find that the pain comes and goes over time. In itself, this is not dangerous or abnormal. The trick is to reduce the discomfort by paying attention to the signals your body is giving you, so that you don’t subject yourself to more pain than you need to – but you should not be
afraid to move.
If you continue to experience pain after your pregnancy, you should discuss the treatment plan with your GP and therapist. Many women benefit from talking to other people who are in the same situation, such as LKB’s peer counsellors.
Aids and equipment if you live in Norway
There are various kinds of aids and equipment that can help you to cope better with everyday life. You should use the aids to relieve strain and prevent pain and discomfort. Aids can be very useful if you are finding it difficult to function for a period, or if you have persistent pain.
If you live in Norway, a doctor, physiotherapist or occupational therapist in your municipality can help you with an application for aids and equipment. They will explain whether you can use the municipality’s short-term supply or whether you should apply through NAV. All municipalities are obliged to keep a supply of equipment for short-term loan to its inhabitants.
Contact your home municipality for more information, your health visitor is often a good place to start.
Examples of useful aids are:
- pressure-relieving pillows
- support cushions for use in chairs and in bed, e.g. breastfeeding pillows
- bean bags
- ‘helping hand’ reachers, for picking up things like toys
- pelvic support belt
- backpack instead of handbag
- microfibre supermop instead of vacuum cleaner
- different types of office chairs
- blocks to raise your bed
- crutches, remember to use ice spikes in the winter and neck strap
- smooth sheets in bed.
Benefits from NAV
- Sickness benefits
- Physical therapy
- Exemption card scheme
- Pregnancy benefits
- Maternity benefits
- Extension of maternity benefits period
- Transfer of maternity benefits to the father
- Care benefits.
If you suffer from long-term pelvic girdle pain, you may be entitled to:
- Work assessment allowance
- Disability pension
- Basic benefit and supplementary benefits
- Benefits towards buying a car
- Stays in rehabilitation institutions.
- BPA – citizen-controlled personal assistance
Physiotherapy
There is no need for a doctors reference to physical treatment. It is, however, important to check that the physiotherapist has a municipal agreement for the exemption card scheme to apply
Transport
If the pain is severe, you may be able to claim for a taxi to take you to treatment sessions and examinations by a doctor, physiotherapist or hospital. You pay patient charges until you reach the maximum annual amount for the exemption card.
There are many benefits that may apply to you, and they are constantly changing. Contact NAV for further information.
Do you need someone to talk to?
LKB’s peer counsellors are women like yourself, with knowledge and understanding. A peer counsellor can share her experiences, and is a woman that you can talk to in confidence. Our peer counsellors are bound by a duty of confidentiality. Find a list of our peer counsellors here.
About LKB – organisation representing the interests of women with pelvic girdle pain
Norwegian Association for Pregnancy-related Pelvic Girdle Health (LKB) was founded in 1987. We are part of and are affiliated to the Norwegian Association for the Disabled (NAD).
LKB has a multidisciplinary panel of experts who assure the quality of the information we provide.
LKB regards preventative work for pregnant women and chronic sufferers as an extremely important focus area. Long-term problems can be prevented if we take action early.
LKB works with the health services and authorities at a national and local level.
LKB’s work through over 25 years has resulted in better treatment and social security entitlements for women and their families.
LKB organises courses and activities for members.
Join LKB
Anyone can become a member of LKB. We need a strong association so that we can present a united front in our work for preventive action and rehabilitation.
As a member, you can
- attend membership meetings
- attend courses
- feel a sense of belonging
- meet other people in the same situation
- have access to our password-protected membership pages at www.bekkenleddhelse.no, where you can find previous editions of LKB-nytt, sound recordings of relaxation exercises and more
- make use of all NAD’s membership benefits
- support the essential work of LKB.
By joining LKB, you are helping to show society how many people are affected by these challenges. Membership of LKB includes membership of the Norwegian Association for the Disabled (NAD).

Telephone: (+47) 24 10 24 00 (NHF service department)
E-mail: post@lkb.no
Website: www.bekkenleddhelse.no
Address: LKB P.O. Box 9217, Grønland NO-0134 Oslo
